FREE! Stop That Clot: Haemostasis and anticoagulants
2 hours
2 hours
Warfarin
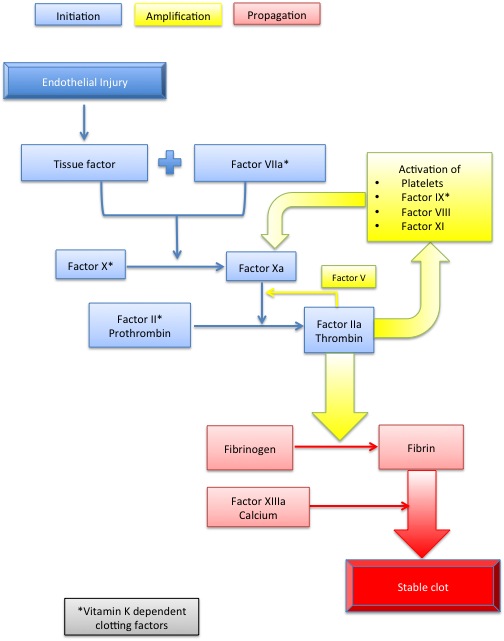
Warfarin is a vitamin K antagonist and, until relatively recently, the only oral anticoagulant available. Vitamin K is needed for synthesis of clotting factors in the liver. In the process vitamin K is oxidised. An enzyme, vitamin K reductase, salvages vitamin K for reuse by the liver. Warfarin inhibits vitamin K reductase (Rang et al., 2012). Many of the essential factors in coagulation are vitamin K-dependant (Figure 3) and so affected by warfarin.Figure 3: Coagulation
Initiation of warfarin therapy in the presence of acute thromboembolism normally overlaps with heparin, for two reasons. First, the full effect of warfarin is not seen until clotting factors already synthesised are removed from plasma (half-life varies between 2 to 3 days). Secondly and more importantly, warfarin affects protein C, an inhibitor of coagulation that also relies on vitamin K for manufacture. It has a shorter half-life (6-9 hours) than the clotting factors (Tanaka et al., 2009). Loss of protein C on initiation of warfarin can cause thrombosis in small vessels of the skin leading to necrosis (Rang et al., 2012).
Warfarin’s other adverse effects pose a significant barrier to use (Neilson, 2010). It has a narrow therapeutic window: the difference in drug concentration between achieving desired effects and inducing toxicity is minimal. Therapeutic effects of warfarin are measured using the international normalised ratio (INR) of prothrombin time (Table 3). In non-warfarinised people, INR is 1. For those taking warfarin, the aim is to establish an INR of between 2 and 3. INR of greater than 4.5 significantly increases the risk of bleeding.
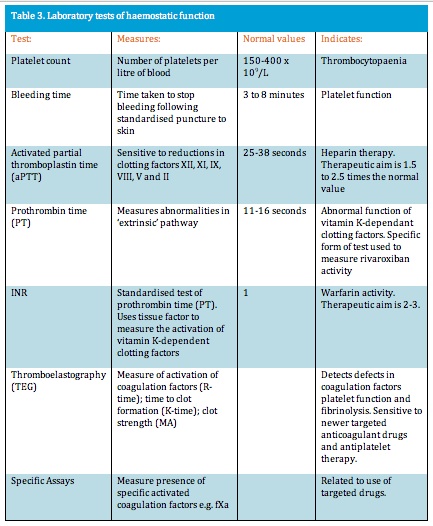
Warfarin is inactivated in the liver via an enzyme system that inactivates many other drugs. Some drugs inhibit the enzyme system, while others induce it. Inhibition by, for example, co-trimoxazole, ciprofloxacin or metronidazole, increases active warfarin, increasing INR and the risk of haemorrhage. Induction of the enzyme system by, for example, St John’s Wort, increases warfarin removal from the body, decreasing INR and increasing risk of thrombosis (Best Practice Advocacy Centre New Zealand, 2007). A more comprehensive list of drugs that affect warfarin activity or metabolism may be found at BPAC NZ.
If a patient on warfarin significantly alters their diet, INR may be affected. Vitamin K is found in leafy green vegetables such as spinach, broccoli and lettuce. Having fresh vitamin K available will allow the body to generate more clotting factors. Vitamin K is fat-soluble so fatty foods increase absorption. Vitamin K is also manufactured in the large intestine by normal bacterial flora. Loss of these bacteria during treatment with broad-spectrum antibiotics can increase the risk of bleeding.
Adverse effects are possible with concurrent use of non-steroidal anti-inflammatory drugs, antiplatelet drugs and particularly aspirin (see below). These have an antiplatelet effect that increases risk of bleeding without altering INR. Aspirin is sometimes prescribed concurrently with warfarin, and patients may self-medicate with this or other over-the-counter drugs and complementary remedies that affect haemostasis.
The need for frequent INR monitoring and follow-up, and significant risk of bleeding make warfarin challenging for patients and prescribers (Witt, 2010). Risk benefit analysis has demonstrated the value of warfarin therapy in AF where risk of serious haemorrhage is outweighed by high risk of stroke. Current guidelines all include tools for assessment of stroke risk and bleeding. The most common are the CHA2DS2-VASc risk score and the HAS-BLED tool.

Initiation of warfarin therapy in the presence of acute thromboembolism normally overlaps with heparin, for two reasons. First, the full effect of warfarin is not seen until clotting factors already synthesised are removed from plasma (half-life varies between 2 to 3 days). Secondly and more importantly, warfarin affects protein C, an inhibitor of coagulation that also relies on vitamin K for manufacture. It has a shorter half-life (6-9 hours) than the clotting factors (Tanaka et al., 2009). Loss of protein C on initiation of warfarin can cause thrombosis in small vessels of the skin leading to necrosis (Rang et al., 2012).
Warfarin’s other adverse effects pose a significant barrier to use (Neilson, 2010). It has a narrow therapeutic window: the difference in drug concentration between achieving desired effects and inducing toxicity is minimal. Therapeutic effects of warfarin are measured using the international normalised ratio (INR) of prothrombin time (Table 3). In non-warfarinised people, INR is 1. For those taking warfarin, the aim is to establish an INR of between 2 and 3. INR of greater than 4.5 significantly increases the risk of bleeding.

Warfarin is inactivated in the liver via an enzyme system that inactivates many other drugs. Some drugs inhibit the enzyme system, while others induce it. Inhibition by, for example, co-trimoxazole, ciprofloxacin or metronidazole, increases active warfarin, increasing INR and the risk of haemorrhage. Induction of the enzyme system by, for example, St John’s Wort, increases warfarin removal from the body, decreasing INR and increasing risk of thrombosis (Best Practice Advocacy Centre New Zealand, 2007). A more comprehensive list of drugs that affect warfarin activity or metabolism may be found at BPAC NZ.
If a patient on warfarin significantly alters their diet, INR may be affected. Vitamin K is found in leafy green vegetables such as spinach, broccoli and lettuce. Having fresh vitamin K available will allow the body to generate more clotting factors. Vitamin K is fat-soluble so fatty foods increase absorption. Vitamin K is also manufactured in the large intestine by normal bacterial flora. Loss of these bacteria during treatment with broad-spectrum antibiotics can increase the risk of bleeding.
Adverse effects are possible with concurrent use of non-steroidal anti-inflammatory drugs, antiplatelet drugs and particularly aspirin (see below). These have an antiplatelet effect that increases risk of bleeding without altering INR. Aspirin is sometimes prescribed concurrently with warfarin, and patients may self-medicate with this or other over-the-counter drugs and complementary remedies that affect haemostasis.
The need for frequent INR monitoring and follow-up, and significant risk of bleeding make warfarin challenging for patients and prescribers (Witt, 2010). Risk benefit analysis has demonstrated the value of warfarin therapy in AF where risk of serious haemorrhage is outweighed by high risk of stroke. Current guidelines all include tools for assessment of stroke risk and bleeding. The most common are the CHA2DS2-VASc risk score and the HAS-BLED tool.
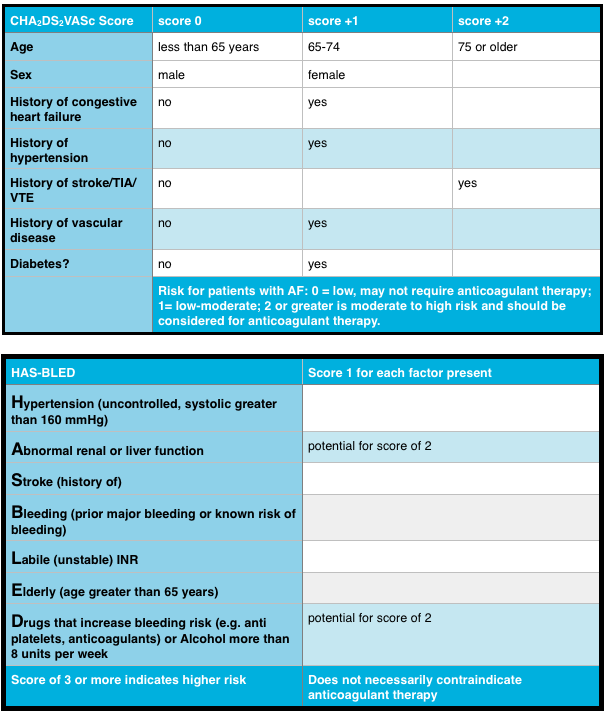
Sources: NICE, 2014; American College of Cardiology, 2014; Lip et al., 2010
The antidote for warfarin in elevated INR or haemorrhage is to administer vitamin K (phytomenadione). This takes some time to have a therapeutic effect; clotting factors or fresh frozen plasma may be needed in acute haemorrhage (Tanaka et al., 2009).